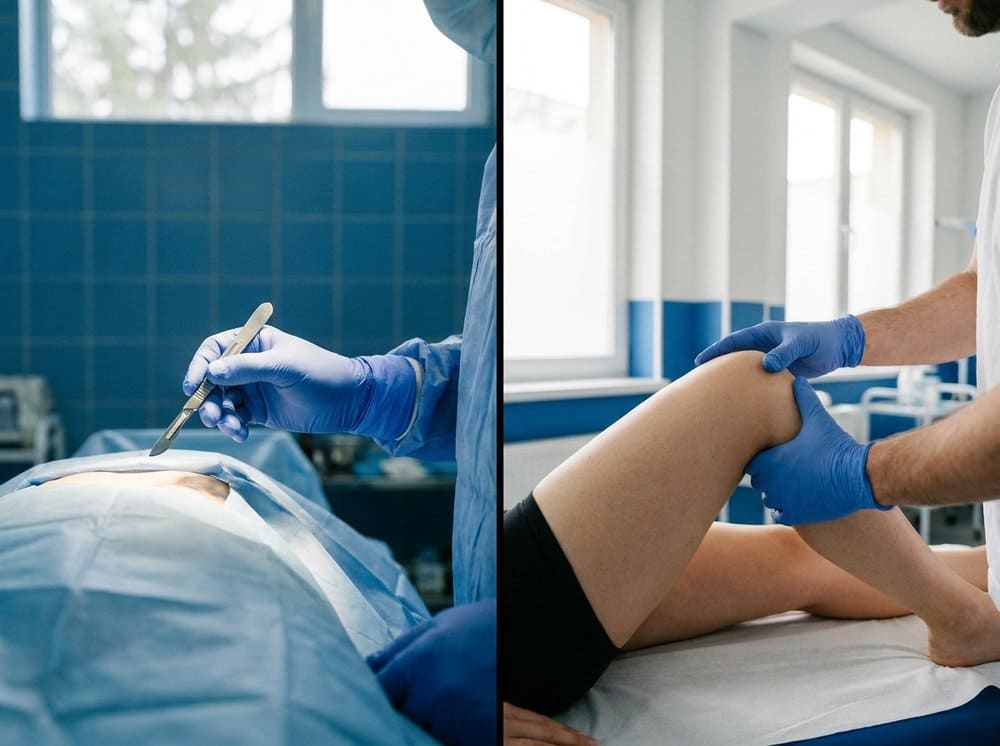
When a patient is referred to our joint injections service, the first conversation is rarely "should you have an injection?" — it is "which one?" Platelet-rich plasma, hyaluronic acid viscosupplementation, and corticosteroid are three legitimate clinical tools with three very different jobs. Presenting them as a single product labelled "knee injection" is how patients end up disappointed: a steroid shot for a biologic problem gives relief for six weeks and then wears off. A PRP series for an acute flare takes four weeks to kick in by which time the patient has been miserable for a month. The match between the drug and the problem matters more than the drug itself.
This article lays out the three options honestly, including the ceiling of each. If you are not yet clear on what Kellgren-Lawrence grade you are working with, start with our X-ray grades explainer — the grade is the single most important input into the decision that follows.
Platelet-Rich Plasma (PRP)
What it is. A concentrate of your own platelets, spun from a blood draw taken on the day of injection. Platelets release growth factors — PDGF, TGF-β, VEGF, IGF-1 — that modulate the local inflammatory environment and may stimulate chondrocyte activity. The injected solution is autologous, meaning it comes from you, which is why the allergic-reaction risk is essentially zero.
Best indication. Early-to-moderate knee osteoarthritis, typically Kellgren-Lawrence Grade I, II, and early III, in patients under 65. The evidence is strongest here: multiple meta-analyses, including a 2021 American Journal of Sports Medicine review, show PRP outperforming both hyaluronic acid and placebo in WOMAC pain and function scores at 6 and 12 months in this group.
Protocol. A series of 2 or 3 injections, spaced 3–4 weeks apart. Each session takes about an hour — draw, centrifuge, ultrasound-guided injection.
Onset. Slow. Most patients notice nothing for the first two weeks, a gradual improvement between weeks 3 and 6, and peak effect around weeks 8–12.
Duration. 6–12 months of meaningful symptom reduction. Repeatable annually.
Cost at Myntrava. ₱12,000 per session. Two to three sessions typical.
Limits. Does not regrow cartilage — no injection does. In Grade IV bone-on-bone knees, the response is weaker and less durable. Not first-line for acute flares because the onset is too slow.
Hyaluronic Acid (HA / Viscosupplementation)
What it is. A synthetic version of the hyaluronic acid that your own synovial fluid already contains. In osteoarthritis, native HA becomes shorter-chained and less viscous; the supplemented HA restores a layer of slippery, shock-absorbing fluid inside the capsule. Some HA preparations also have a secondary anti-inflammatory effect by binding CD44 receptors on synovial cells.
Best indication. Moderate-to-severe knee OA (Kellgren-Lawrence Grade III, and selected Grade IV), particularly in older patients who are not surgical candidates or who wish to delay total knee replacement. NICE guidance is cautious about HA; the OARSI guidelines are supportive for this subgroup. In our practice it is the workhorse injection for the 60+ cohort.
Protocol. A 3-week series: one injection per week for three weeks. A handful of newer long-chain HA products are single-shot, but the 3-week series remains the most common in the Philippine market.
Onset. Moderate. Most patients notice improvement after the second injection, with peak effect 4–6 weeks after the course completes.
Duration. 6–8 months average, occasionally up to a year. Re-course annually or when symptoms return.
Cost at Myntrava. ₱8,000 per injection. Three injections per course.
Limits. Not useful for acute flare control — onset is too slow. Response in younger Grade I–II patients is generally inferior to PRP. Insurance coverage varies by HMO; Maxicare and Intellicare typically cover it with specialist referral, ValuCare and Medicard sometimes cover a portion.
Corticosteroid
What it is. A potent synthetic anti-inflammatory, most commonly triamcinolone or methylprednisolone, usually mixed with a local anaesthetic. It suppresses the inflammatory cascade directly, producing rapid relief but no disease-modifying effect.
Best indication. Acute flare of any grade of knee OA, or as a bridging measure in a patient awaiting surgery or starting PT for whom a week of tolerable movement would change the entire rehabilitation trajectory. Also useful for isolated subacromial, trochanteric, or facet-joint pain presentations.
Protocol. Single injection, occasionally repeated after 3–6 months if indicated.
Onset. Fast. Meaningful relief within 24–72 hours, with peak effect at 1–2 weeks.
Duration. 6–12 weeks typically. After that the effect fades and is not regained by re-injection.
Cost at Myntrava. ₱3,500 per injection, usually covered by HMO with a specialist referral.
Limits — and this is important. Do not exceed three corticosteroid injections per joint per year. Cumulative intra-articular steroid use is associated with cartilage thinning on MRI (Food and Drug Administration communication, 2021) and increased risk of steroid-induced cartilage degradation in long-term observational studies. A corticosteroid injection is a bridge, not a treatment plan. Contraindicated in active joint infection, local skin infection at the injection site, uncontrolled diabetes (blood glucose may spike for 3–7 days), and known allergy.
"The injection should match the problem. A steroid for a biologic question, or PRP for an acute flare, is the wrong tool no matter how well it is delivered."
How we choose, in practice
The decision tree in our clinic is roughly this:
- Acute flare, any grade. Corticosteroid, ultrasound-guided, once. Then immediate enrolment in a structured 12-session osteoarthritis program while the steroid window holds.
- Grade I–II, under 65, chronic symptoms despite PT. PRP series of 2–3 sessions, annual re-course if the response is meaningful.
- Grade III, any age. Usually HA 3-week series. PRP as an alternative for younger patients who prefer an autologous option.
- Grade IV, not yet surgical. HA 3-week series, honest discussion of eventual total knee replacement, supportive PT and lifestyle measures. Corticosteroid reserved for flares.
- Grade IV, planning TKR. We generally avoid steroid within three months of planned surgery (infection risk) and avoid HA within six weeks of surgery. PRP is not contraindicated but offers little benefit at this stage.
All three injections are delivered under ultrasound guidance in our clinic. The ultrasound matters — studies comparing landmark-guided versus ultrasound-guided intra-articular injections find the unguided approach misses the joint space in 15–30% of knees, particularly in obese patients and in Grade III–IV knees where the anatomy is distorted. If your previous injection did not help, the first question we ask is whether it reached the intended target.
What about the other treatments?
Injections do not stand alone. Every patient we inject also gets an individualised exercise plan and nutritional guidance — because the best evidence is consistent: injection plus rehabilitation outperforms injection alone, by a wide margin. Our post-injection rehabilitation track starts 5–7 days after the shot and accelerates the return to normal function. The injection buys the window; the rehab makes the window count.
Questions worth asking your orthopedist
- Which injection are you recommending, and why that one for my grade?
- Is this injection being delivered under ultrasound guidance?
- How long should I expect the effect to last, and what do we do when it fades?
- What is the plan for rehabilitation and lifestyle changes during the effect window?
- What are the red flags I should call the clinic about in the first 72 hours?
A clinician who can answer these cleanly is thinking about your joint as a long-term project rather than a single visit. That is the frame that, more than any individual injection, determines how the next five years of your knee will feel.